Athletes Foot
Athlete’s Foot: Symptoms, Causes, Diagnosis & Treatment
Learn what athlete’s foot is, why it happens, how it spreads, and how treatment (including online consults) can help.
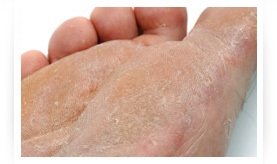
Overview
 The medical term for athlete's foot is tinea pedis, and it's a very common infection of the skin that's caused by a fungus.
Even though the name suggests only athletes get it, it's a frequent misconception as it can happen to anyone.
The medical term for athlete's foot is tinea pedis, and it's a very common infection of the skin that's caused by a fungus.
Even though the name suggests only athletes get it, it's a frequent misconception as it can happen to anyone.
Overall, there's a lot of taboo surrounding athlete's foot since many people associate it with feet uncleanliness. However, that's not accurate since it's a result of a fungus growing on your skin.
When you have athlete's foot, the fungi can grow anywhere on your feet, but it commonly appears between your toes. The bottom of the foot is also often affected, and it can all be very uncomfortable, especially each time you put your shoes on.
Some people believe only one type of fungus is responsible for athlete's foot, but there are many kinds involved. If the fungus comes in contact with your skin, it might probably start to grow, and you may experience different symptoms.
At the same time, you should always get an online prescription for athlete's foot if you believe you have it because it can complicate and cause many more problems. A doctor can diagnose you and recommend the best ways to manage your condition.
If you have athlete's foot, you might feel ashamed or embarrassed. Nonetheless, you should keep in mind that it's a very common skin condition, and it affects more than 15% of the global population. Although it happens to more men than women, anyone can experience it because fungi are everywhere.
The best way to manage athlete's foot symptoms is to identify them, then contact a specialist to help you. Otherwise, you might do the wrong thing, and your feet can worsen.
Signs, Symptoms, and Types
There are four types of athlete's foot: plantar (in the sole of your feet), chronic interdigital (between the toes), acute ulcerative (dangerous lesions with scaly borders), and vesiculobullous (which means you would have fluid-filled blisters).
Even though there are four types, the most common kind is the interdigital athlete's foot, and the fore toe and pinky are usually the ones affected.
In some cases, athlete's foot might not cause any symptoms at first. It completely depends on the type of fungus causing the disease. After some time, your skin might appear scaly, flaky, or it might itch. If that happens to you, you must get an online doctor for athlete's foot as soon as you can.
The least common type is vesiculobullous athlete's foot, but that doesn't mean it can't happen. When it does, it's usually in the sole of your foot, and it causes painful blisters to appear.
You should keep in mind that some types of athlete's foot cause visible symptoms, but you may not experience any discomfort.
However, you still need to contact an online doctor for athlete's foot if that's your case – if you don't, you might experience dangerous complications. Your skin, for example, could crack, which may cause bacterial infections.
Additionally, if your condition spreads, it can reach your toenails and affect them as well. On other occasions, your feet might itch, which is also a problem since it elicits the scratch reflex – if you scratch, you may crack your skin and allow the fungi to grow even further.
People who experience a very severe itching sensation might accidentally inflict excoriations on the skin, also known as open wounds. In turn, that would make your skin prone to bacterial infection, and since you're using your fingers to scratch yourself, the disease may spread under the fingernails as well.
Common symptoms
- Itching, burning, or stinging (especially between toes)
- Scaling, peeling, or flaking skin
- Redness, cracks, or painful splits in the skin
- Blisters (in some cases)
- Possible spread to toenails (thick, discolored nails)
Diagnosis and Tests
If you want to get an online doctor's prescription for athlete's feet, you need to contact a professional first. Then, they might probably follow the standard procedures, for example, asking for your medical history.
The doctor has to check your medical history to determine risk factors that might have intervened in you getting athlete's foot. Furthermore, they may conduct an interview to know more about your reactions to it, especially to identify whether you scratched your feet or not.
In many cases, patients don't want to admit they scratched their feet because it makes them feel embarrassed. They might believe the condition worsened (or even appeared) just because of that.
However, you should keep in mind that itchiness is a common symptom of athlete's foot, and the scratch reflex is sometimes automatic, which means you can't always control it. All doctors understand it, and the reason why they want to know more about your case is to determine the right treatment for you and help you get better.
After the interview, the doctor might conduct a short physical examination. In most cases, an experienced professional is able to diagnose the condition right away since the visual signs of athlete's foot are very specific.
Nonetheless, sometimes, the diagnosis is uncertain. If that happens, the doctor may recommend a KOH test (a specialized evaluation method), which helps rule out psoriasis, candidiasis, contact dermatitis, and similar skin conditions.
Some people believe the doctor can diagnose athlete's foot by using a UV lamp, but that's not the case. Unlike other kinds of fungi or bacteria, the fungus that produces this skin condition does not fluoresce under UV light.
Treatment, Medications, and Care of Athlete's Foot
Even though experiencing athlete's foot is very uncomfortable and can hinder your life, there is a treatment for it, which is why you should contact a doctor to help you.
Athlete's foot can not only cause nasty symptoms, but also make you feel pain or discomfort when you're putting your shoes on or walking. In turn, that might provoke negative feelings, such as shame, embarrassment, or even anxiety, especially if you have to let other people see your feet.
On some occasions (around 30% to 40% of cases), athlete's foot improves on its own when you follow the doctor's suggestions. The professional might recommend you wash your feet twice a day, and then apply some topical medication.
Consistency is key once you start your athlete's foot treatment, especially at the very beginning of it. The process doesn't last for months, so making sure you follow the doctor's orders is vital if you want to improve, even after the symptoms disappear.
Your outer skin is susceptible to becoming infected again if you don't properly take care of it, which is why you should also make sure you follow the doctor's suggestion even if you believe you're cured. In other words, they might instruct you to continue with the treatment for two to six weeks after the symptoms stop, but it's often to prevent it from appearing again.
Furthermore, sometimes treating your feet is not enough, especially if you're used to wearing socks. To disinfect them, you can wash them in water at 140 degrees Fahrenheit or use bleach.
Nonetheless, keep in mind that there's no way to know whether or not your shoes still have the fungi, and if you want to be completely sure, you have to dispose of them.
At the same time, if you've scratched your feet, you're probably going to have to apply the medication on your hands as well – the same goes for any other part of your body where the fungus might spread. If you don't treat it, it can keep growing even if your feet don't have it anymore.
Lastly, if your infection is severe or keeps reappearing, you might have to take some oral medication for it as well.
Living with Athlete's Foot
The name of this condition started appearing due to its prevalence among many athletes, but it can happen to anyone – there are fungi all around you right now, and you can even have them on your salad without realizing it.
Even though it's immensely common, some people avoid going to the doctor because they feel very ashamed, which might cause their skin to worsen and the fungus to spread to other parts of their bodies.
Consequently, you should keep in mind that the best way to deal with it is getting an online prescription for athlete's foot. The doctor can evaluate your symptoms, determine the type of fungus spreading on your skin, and recommend the best treatment for it.
Moreover, you must be consistent if you want your skin condition to improve. Just like with other skin problems (such as acne), you have to follow the doctor's suggestions regularly, otherwise, you can't see any change.
Athlete's foot can hinder many people's lives, especially if they're in pain, if they have blisters, or if they have open wounds. Therefore, you shouldn't wait if you believe you have it – contact a doctor as soon as you can.
Remember that some types of fungus may not cause discomfort, but you should still deal with the condition if you don't want it to worsen or spread to other parts of your body, for example, your fingernails, hands, or even your torso.
With a prescription online for athlete's foot, you can slowly recover your skin's usual beauty, but you need to get help and follow the doctor's orders.
Frequently Asked Questions (FAQ)
1. What exactly is athlete’s foot?
Athlete’s foot (tinea pedis) is a fungal infection that affects the skin of the feet—most commonly between the toes and on the soles. It can cause itching, burning, scaling, redness, and cracking.
2. What causes athlete’s foot?
It’s caused by fungi (dermatophytes) that thrive in warm, moist conditions. Walking barefoot in shared showers, locker rooms, and pool areas—or wearing sweaty shoes—can increase risk.
3. How can athlete’s foot be treated?
Treatment typically uses antifungal medications. Mild cases may respond to OTC creams, powders, or sprays, while persistent or severe infections may need prescription-strength topical or oral antifungals.
4. Can I get an athlete’s foot prescription online?
Yes. Many online medical services allow a virtual assessment and, if appropriate, can provide a prescription antifungal medication sent to your pharmacy without an in-office visit.
5. What medications are used to treat athlete’s foot?
Common treatments include topical antifungals such as terbinafine, clotrimazole, ketoconazole, or ciclopirox. In resistant or widespread cases, a healthcare provider may recommend an oral antifungal.
6. How long does athlete’s foot treatment take to work?
With consistent treatment, symptoms often improve within 1–2 weeks. Many plans continue for several weeks to make sure the fungus is fully cleared and to help prevent recurrence.
7. Are there things I should do at home to help treatment work?
Yes. Keep feet clean and dry, change socks daily, wear breathable shoes, and avoid walking barefoot in public damp areas. These steps support healing and reduce reinfection risk.
8. Can athlete’s foot go away without medication?
Mild cases may improve with good hygiene, but antifungal treatment is usually much more effective and helps prevent spread to nails or other areas.
9. Is athlete’s foot contagious?
Yes. It can spread through direct contact with infected skin or indirectly from contaminated floors, towels, socks, or shoes. Treating it and practicing good foot hygiene helps reduce spread.
10. When should I see a healthcare provider about athlete’s foot?
If symptoms don’t improve after a couple of weeks, the infection spreads, or you have diabetes or a weakened immune system, seek medical evaluation. Prescription treatment or further care may be needed.

WARNING: Limitations of Online Doctor/Medical Consultations and Online Prescriptions, QuickRxRefills Cannot and Will NOT Prescribe, Dispense, or Resell any and all medications Narcotics/Controlled Substances (this policy is fully enforced by the Drug Enforcement Administration (DEA)) for Anti-depressants, Pain, Anxiety, Weightloss, Sleep, ADHD/ADD, Anabolic Steroids, Testosterone Replacement Therapy and any and all Medications that contain GabaPentin or Pseudroephedrine including non-controlled substances or any medications that are considered controversial, Off Labeled (Growth Hormone aka HGH) or recalled in nature such (i.e. Retin-A, Accutane). Furthermore, QuickRxRefills is not a substitute for an office based physician in your location nor is it a substitute for Emergency Medical Care or 911. If you do experience a "true" medical emergency your are encouraged to pick up the phone and dial 911 as soon as possible.






